Thank God I’m home. I can’t express the relief I felt on the afternoon of Monday the 18th of May when Anna and my friend Cansun (see earlier post) came to pick me up from St Mary’s and delivered me back here – where Maddy soon joined us after nursery. It’s been such a tonic to see her after so many days apart. (Anna and I thought it best to spare her the experience of a hospital visit – it’s disorienting enough for grown-ups – at best, we feared, it would confuse and, at worst, terrify.)
Maddy was a little wary at first, seeing me slumped like a sack on the sofa, still winded by the exertion of climbing the stairs twenty minutes earlier. She knows I’ve been ill and in hospital but she’s not been sure what it means, except for further disruption in her routine. But she very quickly warmed up and I knew I was really on the mend the moment she performed the welcome home daddy routine she’d evidently been learning during my week in hospital. Imagine her sashaying across the living-room, shoulders shuffling one way, hips the other, hands spinning round each other to the front – all accompanied by lots of laughter as she sang:
‘Shik-a bam, bam, daddy,
‘Shik-a, shik-a, bam, bam.’
Then at last she fell into my arms without any constraint. Nothing so healing as a three-year-old’ cuddles and a daughter’s insistence that ‘daddy, you’re a silly-billy’ because I laughed so much, despite the excruciating toll on my stomach wounds. Worth every stab.
After vomiting first thing Tuesday morning, I felt progressively better physically as the day wore on. I had real pain only when I coughed or sneezed or laughed (all scrunching up my wounded abdominal muscles) and was able to start cutting back on the paracetemol I’m supposed to be taking in industrial quantities (though in my opinion, it’s largely a placebo). I was able to eat a little and often and to begin to take my old random interest in everything around me, from a book my friend Nick gave me on the Last Supper to the weather, to the new ‘smart’ t.v. which Anna’s given me as a wedding present and Maddy’s adventures at nursery.
On Wednesday the 20th, my brother Ames arrived from California, providing another huge boost. Somehow his very presence gives me an extra source of confidence, as if he’s reverting to the (occasionally!) protective ‘big bro’ of childhood. He’s not only very strong physically, but also emotionally, and I know that I can rely on him 100% during the ups and downs which doubtless lie in wait as my recovery continues. He’s also one of the best-informed and most left-field-thinking people I’ve ever known and I know he’s going to provide me with huge mental and intellectual stimulation, too. Indeed, our lengthy conversations are one reason that this post has been delayed
Despite these very positive developments, which include my first walks outside the flat and repeated negotiation of the many flights of stairs within, I still feel traumatised by my period in hospital, from 12-18 May. Sorry if what follows is tedious and self-absorbed (EGO) but I need to write it out to help me let go and move on. Thinking back to some of the things I wrote before the op makes me feel that I was somewhat self-indulgently callow about what was coming up. I think I was partly seduced by a certain Romantic glamour in the idea of premature death, fed by knowledge of too many artists and literary characters whose lives were cut short (usually a lot shorter than mine might be). I guess the mood of much of what I wrote is encapsulated in Keats’s wonderful line from the ‘Ode to a Nightingale,’ – ‘I have been half in love with easeful Death’ – words penned when he was already sick with the TB which would carry him away. A few days in St Mary’s established quite another thematic, the protagonist’s agonised lament in Marlow’s Dr Faustus: ‘Why this is hell, nor am I out of it.’ I think St Mary’s rubbed my nose into a reality that Keats’s Romanticism manages so brilliantly to both absorb and transcend in a manner well beyond my limited powers.
Don’t get me wrong. I know that the operation and a spell hospital are essential steps towards giving me a fighting chance of seeing this thing off. I also know that many people have to suffer far worse than I did. And I freely acknowledge that I had some amazing people looking after me. I want to record my profoundest thanks to my surgeon’s team (an Iranian, a Jordanian Palestinian and a British Muslim woman – are you listening Nigel Farage?) and some of the nurses who helped me afterwards, especially Francis Kennedy, Christina Gomes, Jack Marchant, Tiggy and Clara. You couldn’t have done more…
And yet, and yet…
My first feelings of discomfort began with the epidural before the op. Bent over a cushion to produce the correct curvature of the back, I wanted to be sick as the long needle crunched its way through the cartilage round the spine, not once, not twice, but three times as the anaesthetist sought the best place to deliver maximum relief. The sound was like a chicken wing gristle being torn off the carcase.
Covered with tubes as I already was, I remember nothing after the epidural until I woke 4-5 hours later in the recovery ward at St Mary’s. The tubes had multiplied and any movement seemed to bring protesting pricks from different parts of my body, the canulae on the back of each wrist for antibiotics and saline, the ‘central line’ attached into the side of my neck which managed the pain relief, the catheter attached to my urethra, the drain tube below the stomach wounds, still removing fatty blood from the internal site of the cutting into a colostomy-type transparent bag, the oxygen tube feeding both nostrils, the tube into my spine topping up the epidural, the discomfort of the two lines of clips holding my guts together. Nothing for it but to lie completely still, only my eyes moving, trying to understand what the nurses were telling me.
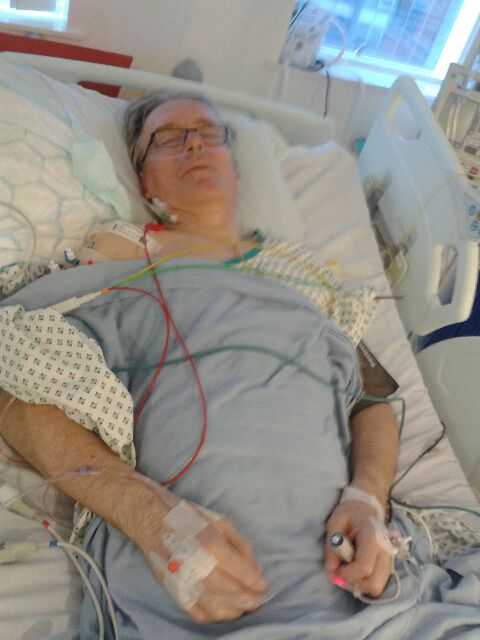
I was being moved to a high dependency unit. There’d been a problem with the surgery. On opening me up, Mr Khoubehi discovered that my right kidney had become adhered to the diaphragm and lung (a process which Ames tells me could only have happened over a very long period of time.) The solution was to cut higher up than planned, partly through the diaphragm and very, very slowly, tease the kidney off the lung in order not to damage the latter. That all went fine. The problem was that cutting higher took the team beyond the band of midriff for which the epidural had been calculated to be sufficient. The consequence was the need for much higher doses of pain relief, especially the synthetic morphine equivalent, fentanyl.
For the first day or so, this provided a fair amount of trippy fun. I can remember joking a lot with Anna, the nurses and other patients, in-between blank periods of sleep and / or unconsciousness. The trouble began when, after a day or so, I was moved to a normal ward, where the fentanyl dosage started to make me vomit a noxious orange, extremely acid, viscous effluent, causing pains in the abdomen which even the fetanyl seemed unable to suppress and the very memory of which makes me want to gag again.
By this stage, I was managing my own pain relief through PCA (patient-controlled analgesia) delivery into a canula. The only solution seemed to be to cut it right down and substitute oral pain-killers of industrial strengths. These, however, made me sicker than ever, so I decided to refuse them, too, unless the pain got unbearable.
It was following that decision that it felt like I’d fallen off a cliff into an abyss which I soon simply couldn’t see myself climbing out of. In retrospect, I guess it was coming off all the pain-killers too quickly, without ‘stepping down’ in the usual manner. Whatever, I was afflicted with such utter feelings of worthlessness that I was often in tears. The self-loathing was compounded by further feelings of self-loathing that I was reacting so irrationally / self-indulgently, when I knew it would eventually pass. But nothing could shake the dark shadow off and Anna’s daily visits provided only temporary relief. Once she was gone, I didn’t even have the strength to do my daily visualisation exercise of seeing Maddy at her graduation ceremony, something I’d been doing for some time at Ames’s suggestion. I couldn’t find the heart even to switch on the Ipad and participate in some of the meditation exercises Sally and Gabi had introduced me to. I just lay there in a stupor of abject misery, unable to eat, immobilised, incapable of any sort of positive thought.
When you fall into this state, hospital’s most definitely not the place to be. A more sterile and denatured environment can hardly exist. The temperature in the ward’s kept artificially constant, day and night. Through the tinted outside windows it’s impossible to tell the weather, unless the sun is shining brightly. The lighting is on 24/7, only being dimmed, not extinguished, at night. One day I fell asleep at bout 5 in the afternoon and woke at 8.45. Convinced it was morning, I struggled upright. I almost burst into tears when I realised I’d been asleep less than four hours and the whole awful night which I thought was past in fact still lay ahead. The food is disgusting beyond words and extremely monotonous, the difference between lunch and dinner menus negligible.
Imagine forever waking and seeing a row of four fellow-victims opposite. Often, everyone’s asleep, on their backs, mouths open, snoring more or less noisily. Knowing you present the same unedifying spectacle to them is not good for self-esteem. In the far corner was Carlos, a Chilean recovering from prostate surgery. His expression permanently startled, and fearful, Carlos barely inter-acted with anyone else, burying his nose in one Marguerite Yourcenaar novel after another. Next to him was Brian, who was in a terrible state, his skin wrinkled and fissured, like a diabetic denies insulin. Unable to speak, Brian could only communicate with grunts. Yet a sweetness always shone in his eyes. The moment I arrived, he gave me a thumbs-up; and that became the gesture with which we always communicated. Most heart-breaking was that Brian never had a visitor in the time I was there. I can’t imagine how he is going to cope once he’s released.
The other two beds opposite were occupied by people on shorter stays; a Kurdish man who drove Brian to distraction because of the huge and hugely noisy caravan of relatives who visited him, despite constant reminders from the nurses that only two people were allowed at a time; an immensely obese man who’d had his bowel removed some time ago but had been run into by a kid on a bicycle, causing the suturing to burst; an elderly Irish carpenter who spent his time rustling noisily in the many plastic bags he’s brought with him; another elderly man who joked that he knew his enema would only work once in the taxi he’d ordered to take him home. The single other bed on my side was occupied by John, the only one of us who appeared to be able to stomach the food, eating his way methodically through every menu, much to my involuntary disgust as the smells floated across.
Above all, in hospital one can barely string more than a few hours sleep together. The interruptions are constant and implacable. From 8 am, there’s a perpetual round of taking of patients’ blood pressure, of their temperature, of siphoning off their ‘bloods’ for testing, of administration of medicines, of doctor’s visits, of blood-thinning injections, of ‘meals,’ of bed-changing. I estimate fourteen to fifteen interruptions every day up to midnight. Then, if you have the ill-luck to be situated adjoining the nurses’ station, as I was, there’s constant noise throughout the night, chatting, laughter, the arrival and departure of patients, of trolleys, the call signals to nurses, the phones ringing. You get more and more exhausted every hour you spend inside.
Little wonder that by the sixth morning of my stay, the Monday I came home, I was at the end of my tether. I spent twenty minutes retching into one of the paper bowls provided for the purpose, watched indifferently by a nurse at the central station. Once she’d finally shuffled over to dispose of the thing, I forced myself out of bed, waddled down the far corridor, phoned my friend Gabi, the counselling psychologist and broke down completely, barely able to say a word through my sobs.
Yet her patient listening and encouragement proved the turning point. Somehow, the tears helped vent the psychological burden as surely as the final bout of vomiting had purged most of the remaining poisons raging inside my body. By the time my surgical team arrived, I felt calm again, reassuring them I was ready to be discharged. The only obstacle remaining was that, after a whole week, I still hadn’t ‘emptied my bowels.’ They didn’t like that, even though ‘timely discharges’ is identified all over the ward as that month’s ‘customer-service’ target. I was sent for an x-ray to make sure there hadn’t been a blockage. Perhaps it was the x-ray because, thank God, my body at last responded, just before lunch-time, even if only a few miserable sheep’s pellets. I was free to go. I couldn’t help my elation.
‘Tiggy,’ I grinned, ‘I’ve had a shit.’
The student nurse grinned back, completely unabashed by my language.
Looking back now, from a vantage point where I’m not taking any form of medication, I realise that the intense depression I felt during my last few days in hospital was largely a chemical reaction. I can scarcely believe what I had pumped into me: epidural, general anaesthetic, fentanyl (synthetic morphine), anti-vomit medicine, blood-thinning agents, eight paracetemol tablets daily, anti-constipation agents (Movicol laxative twice daily and senna pod tablets nightly). Yuk, Yuk, Yuk. The effects on the body are staggering. 62 years of regular peristalsis come to a complete halt as your bowel has simply ‘forgotten’ how to ‘open the bowels.’ The first time I got out of bed, it was as if I was having to learn to walk all over again. My legs were so heavy I could hardly move them, my sense of balance so compromised that I had to cling to Anna for support.
But equally difficult were the psychological effects of the total loss of independence. I didn’t even have ownership of my most basic bodily functions. Being ‘encouraged’ on a regular basis to go and ‘open your bowels’ is hardly agreeable in any circumstances; but when you’re dragging your catheter along on a tripod for company to the airless, window-less latrines, where the smell of the chemicals being used to keep them clean makes you want to gag, it becomes near-impossible. The final humiliation was the enema I was given to try to jolt my bowels into action. Not so much the intrusion into a part of the body which no-one ever gets to see in normal circumstances, though that’s bad enough, but the nappy you have to wear afterwards, ‘just in case’ you don’t make it to the loo quickly enough. As the nurse taped that nappy on, I felt that one can’t fall any lower.
I guess what really surprises me, in retrospect, is how little the NHS seems attuned to the psychological consequences of an operation. Several mornings running I told my nurses I felt helplessly depressed and needed some help. They all seemed surprised, though they must come across this all the time, if my friends who’ve had operations are to be believed. One after another, they’ve been telling me of the abysses they, too, slipped into, sometimes for weeks after their ordeals. Yet there is absolutely no support when you get into this state.
Looking back now, four days after arriving home, I am now really beginning to put this ordeal behind me. I can even laugh at myself in the cartoons my dear friend Janice in New York has sent me.


I can rejoice being back with Anna, Maddy and my brother Ames, I’m eating well, I can take an occasional turn round the roof-deck, and am starting to contact friends again. I’m also fortified by the knowledge that in so much of classic literature, the protagonist has to go down into the underworld as part of the journey towards renewal and enlightenment. So even if I am gagging with relief to have managed to get out of my particular Hades, I’m not going to forget it in a hurry. It’s taught me valuable lessons which I’ll come back to in the final post of this part of the blog.
Apologies if this post has had a somewhat downbeat tone and the prose has been a bit turgid and stiff or more than usually formal. It’s been difficult looking back, but writing in this detail about hospital has really helped me put things in perspective. My old self is rapidly reforming. I’m regaining my robust sense of pleasure in life and thoroughly enjoying my beloved family. And I’m more determined than ever to beat this thing. I haven’t gone through Hades just to let this disease conquer me further down the line. Underpinning that determination is a further major, major development which I will share with you in the next post…
You’re torturing us with the suspense. Can’t wait to hear about the big big development.
It’s horrible that you had such a hateful hospital stay. Much the same everywhere and for so long. Crazy that it has to be thus.
So glad you are home & that your family is with you. As are all of us in spirit. xxoo
LikeLike